New Research Unveils Breakthrough for Lung Cancer with Brain Metastases
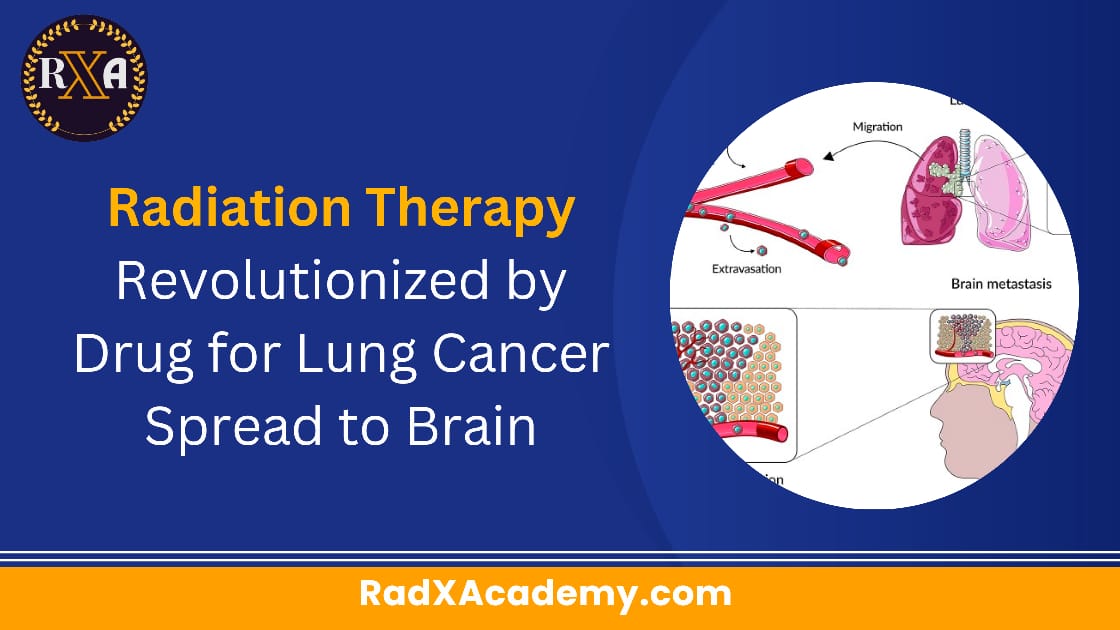
A pioneering study led by researchers from the University of Cincinnati has unveiled a potential game-changer in the treatment of lung cancer that has spread to the brain. This groundbreaking research, recently published in the journal Cancers, sheds light on how a novel drug, AM-101, can amplify the effectiveness of radiation therapy, offering new hope to patients.
Lung Cancer and Brain Metastases: The Challenges
Lung cancer remains the leading cause of cancer-related deaths in the United States, with the American Cancer Society noting that it accounts for one in five cancer fatalities. Non-small cell lung cancer (NSCLC) is the predominant form of lung cancer, representing approximately 80% to 85% of all cases. Alarmingly, up to 40% of lung cancer patients develop brain metastases during their illness, with a typical survival period of only 8 to 10 months after diagnosis.
Currently, standard treatments for lung cancer brain metastases include surgical resection, stereotactic brain radiosurgery, and whole brain irradiation (for patients with more than 10 metastatic brain lesions). However, these treatments often come with significant challenges. “Lung cancer brain metastasis is usually incurable, and whole brain radiation treatment is palliative, as radiation therapy is limited by toxicity,” explains Dr. Debanjan Bhattacharya, the study’s lead author and a research instructor at UC’s Department of Neurology and Rehabilitation Medicine.
Managing radiation’s side effects and overcoming resistance are critical hurdles in treating such cases. The need for less toxic, cost-effective therapies that improve radiation’s efficacy while enhancing patients’ quality of life has never been greater.
The Promise of AM-101
Bhattacharya and his team directed their research efforts toward AM-101, a synthetic analog in the benzodiazepine drug class. Initially developed by medicinal chemist James Cook, the effect of AM-101 in NSCLC was previously unexplored. What makes AM-101 particularly promising is its ability to penetrate the blood-brain barrier, a protective shield of the brain that often blocks drugs from reaching their target.
How AM-101 Works
The research discovered that AM-101 activates GABA(A) receptors present in NSCLC and brain metastatic cells. This activation initiates a process known as autophagy, where cells degrade and recycle unwanted components. Specifically, AM-101’s activation increases the expression and clustering of GABARAP and Nix, two autophagy receptors, effectively enhancing this “self-eating” process. As a result, lung cancer cells become more vulnerable to radiation therapy.
Research Findings and Impact
Using animal models of lung cancer brain metastases, the study revealed that AM-101 significantly enhances the effectiveness of radiation therapy, improving survival rates. Furthermore, the drug slowed the growth of primary NSCLC cells and brain metastases. Combining AM-101 with radiation could also allow for lower radiation doses, reducing side effects and toxicity for patients.
The team is now working towards Phase 1 clinical trials to test the combination of AM-101 and radiation therapy in treating both primary lung cancer and brain metastases.
A Collaborative Achievement
This research represents a collaborative triumph, involving contributions from multiple academic institutions and shared university research resources. Bhattacharya began the project under the mentorship of Soma Sengupta and Daniel Pomeranz Krummel, former UC researchers now at the University of North Carolina at Chapel Hill.
“The entire work, along with revision experiments, was done at the University of Cincinnati, reflecting strong collaboration between multiple teams,” Bhattacharya shared. He dedicates this breakthrough to his late father, whose passing in 2021 inspired him to persevere with the study. “My father’s passing motivated me to work harder to complete this project, as he had known about my research and wanted to see me succeed.”
Looking Ahead
The findings from this study mark a significant step toward improving treatment outcomes for patients with lung cancer brain metastases. The promising results of AM-101 combined with radiation therapy provide a beacon of hope for more effective, less toxic cancer treatments in the future.
Reference : Radiation for lung cancer that has spread to the brain